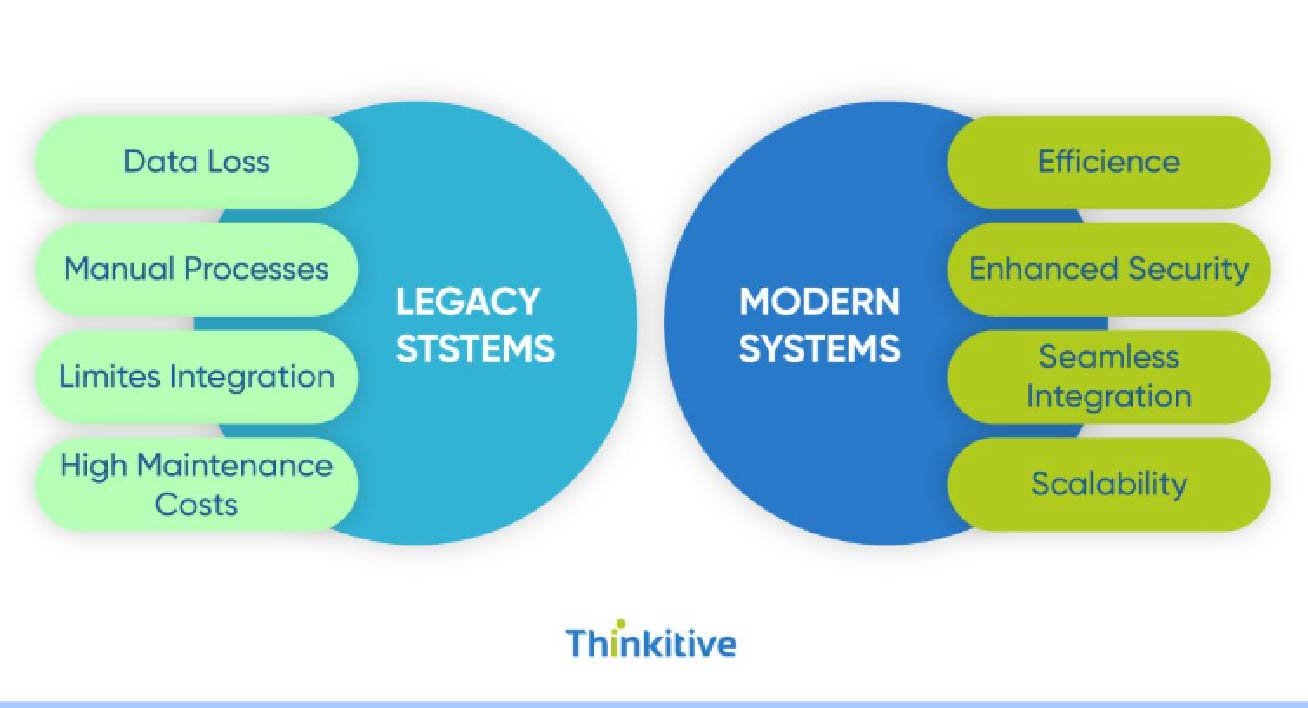
Custom EHR Implementation Case: From Legacy to Modern System
We have been serving the healthcare IT industry for a decade, and we can say that healthcare systems have become much more advanced than they were a decade or two ago. And while we can see a trend of digital transformation in the healthcare industry, several studies imply 60% of the healthcare providers still use legacy systems.
While the legacy systems are strong, a slight difference in those systems can make your EHRs slow, which has a trickle-down effect that slows the clinical and administrative speed of your healthcare practice.
Moreover, given the nature of the healthcare industry, both the technological landscape and regulatory landscape are rapidly evolving. To be able to adapt to these technologies, healthcare practices must move on to modern systems.
And that has been the recent demand in the healthcare industry, seen sharply. You see, most of the projects we are attracting are EHR custom software development. But the concerns about practices in adopting technologies are also genuine. Most of the practices fear data loss, downtime in practices, and disruption of workflows.
However, they are wrong!
You see, it all depends on your EHR modernization and legacy EHR migration of data. In simple words, there won’t be any data loss if you have a structured legacy EHR migration approach. These approaches eliminate risks and give your system a completely modern outlook with necessary customization that improves efficiency and financial performance.
And our latest project is proof of that. In this blog, or rather a case study, we’ll see the implementation of a custom EHR software and how a practice transformed its systems from legacy systems to modern systems.
So, without further ado, let’s get started!
Why Sticking With a Legacy EHR Hurts Practices
Before deep diving into the case study, we first need to understand the root cause behind this EHR modernization, the need to migrate legacy EHR systems to modern systems. Here are some reasons that you need to know:
- Compliance Needs: HIPAA-compliant EHR systems are in high demand in healthcare practices. You see, the legacy systems still adhere to outdated HIPAA regulations and previous FHIR/HL7 integration standards. To adhere to these needs and evolve at their own will, many practices are looking for custom EHR development.
- No FHIR/HL7 Support: Many practices adhere to the outdated standards of FHIR/HL7 integration standards. While the support for these standards is still there, many systems work faster with the latest technology, as modern integrations for lab imaging and telehealth require that.
- Slow & Outdated UI: One of the major concerns of practices is still the use of outdated UI. And it’s true that many practices have a very boxy UI, which makes their use boring. With custom EHR development, you can even improve the UI and curate the workflows in a way that reduces workloads and burnout chances of both clinicians and administrators.
- Vendor Support: Due to the incompatibility of legacy systems with modern systems, the vendor support becomes slower, since it takes more time in implementation and changes. And due to the increased workload, it also increases the cost of maintenance. To avoid providing proper vendor support is necessary.
Case Study Snapshot: Legacy EHR Migration Done Right
The project we talked about in the introduction was very interesting. The clinic was a mid-sized practice that wanted to upgrade its 10-year-old EHR system. Here is a quick snapshot of what we did for their EHR modernization and to migrate their legacy EHR.
- Initial Challenges
The client faced a higher rate of denial, which was almost as high as 20%. Coupling with that, the rigid system increased the patient check-in time by almost 10 minutes. Due to the backlogs from the start, poor reporting, with almost zero analytics reports, was formed. Upon close inspection, we realised that this was due to a manual process as their EHRY systems were disconnected from the billing and lab systems.
- Custom EHR Development Strategy
We divided the development strategy and integrated the healthcare data migration steps into that as well. Here are some of the steps in which we divided the development strategy:
| Phase | What Happens in This Phase |
| Phase 1: Discovery & Data Mapping | Legacy workflows and databases were assessed to plan legacy EHR migration and align data with modern EHR structures. |
| Phase 2: Secure Data Extraction & Cleansing | Patient records were securely extracted and standardized as part of a compliant healthcare data migration strategy. |
| Phase 3: Custom EHR Development with Modern Workflows | The system was rebuilt through custom EHR development, focusing on usability, scalability, and EHR modernization goals. |
| Phase 4: Migration, Validation & Parallel Testing | Historical data was validated as teams migrate legacy EHR data and test interoperability, including FHIR/HL7 integration. |
| Phase 5: Go-Live with Staff Training | The new platform was launched as a HIPAA-compliant EHR system, supported by structured staff training and transition support. |
- Real Results
The staggering result that we achieved with this custom EHR development strategy transformed the practice. For instance, the denial rate was brought down to 50%, and the time required for patient check-in was minimized to 3 minutes. Of that, 99.9% of the data integrity was maintained after legacy EHR migration, enabling smoother workflows and increasing clinician satisfaction to a new high.
Key Strategies for Successful Migration
There were some key strategies that we implemented for successful healthcare data migration for this practice. Here is a short sneak peek into our strategies:
- Data Cleansing & Validation: Before moving to the newer system, we transformed the data into the proper structure by cleansing and validating it for the right standards.
- Removal of Unnecessary Data: We noticed that most of the data that was stored was excessive in nature. Then we filtered which data was required for migration and which needed to be archived. This makes the process much easier, and only the important aspects were integrated into the system.
- Rigorous Testing: After the data was migrated, we rigorously tested the data for legacy systems and new systems so that all the aspects of the system were up and running, without creating disruptions in the clinical and administrative workflows.
- Parallel Go-Live: One of our best practices includes running the rollout strategy in parallel with development. This way, a safe rollout was ensured, and necessary changes were made in the system in real-time.
Choosing the Right Migration Partner
Your legacy EHR migration relies mostly on the partner you choose for your healthcare data migration and custom EHR development. And this is where most of the practices go wrong. Here is a quick guide to help you choose the right legacy EHR migration:
- Proven Experience: Work with or choose the development partner who has proven experience in custom EHR development. This is important to cover all the important aspects in custom EHR development and legacy EHR migration. Also, the additional benefit you get is elevated development speed.
- Compliance & Requirement Understanding: There are various compliance and local and federal requirements that you need to adhere to. For this, your partner must have an in-depth understanding of HIPAA, FHIR/HL7, and healthcare compliance. This helps develop a HIPAA-compliant EHR system.
- Risk Handling: Another important quality that you need to consider in your custom EHR development partner is their ability to handle data security, auditing, and migration risk. These are risky yet important steps in legacy EHR migration, and they need to be done carefully to avoid data loss.
- Long-Term Support & Maintenance: You are going to use this EHR software for a long period of time, and during that time, both the healthcare and technological landscapes are bound to evolve. That is why it is important to choose a partner who provides you with long-term IT support and helps in the maintenance of your system even after deployment.
Conclusion
In this way, we developed a custom EHR system and transformed the practice by implementing the right legacy EHR migration strategy. Due to this, the practice was able to streamline and fasten its clinical, administrative, and financial operations.
If you are a provider, let this blog be the blueprint for your EHR modernization, and I hope I convinced you why you need the right partner for this process. Practices need to modernize their system in a safe environment and not disrupt the efficiency or current day-to-day functioning of the practice in that process.
So, are you still using the outdated system? Change that with our EHR modernization strategy, and click here to understand how we can do it for you.
FAQs
- How long does a typical legacy EHR migration take?
The timeline for a legacy EHR migration typically ranges from 8 to 24 weeks, depending on system complexity, data volume, and integration requirements. Smaller practices with structured data may complete migration faster, while enterprise or multi-location systems require more time for validation and testing. A phased approach—starting with discovery and data mapping—ensures smoother EHR modernization without disrupting clinical operations.
- Will we lose data when moving from an old EHR to a new custom system?
No, when executed correctly, healthcare data migration is designed to preserve 100% data integrity. Structured data (clinical notes, medications, labs) and unstructured data (documents, scanned files) are carefully mapped, cleansed, and validated. Parallel testing and reconciliation processes ensure nothing is lost when you migrate legacy EHR data into a modern, purpose-built system.
- Can a custom EHR integrate with our existing labs, billing, and telehealth tools?
Yes. Custom EHR development enables seamless integration with third-party systems such as labs, imaging centers, billing platforms, and telehealth tools. Using industry standards like FHIR/HL7 integration, a modern EHR can exchange data in real time, reduce manual entry, and support interoperability across your healthcare ecosystem—without replacing tools that already work well for your team.
- Is the migration process HIPAA-compliant and secure?
Absolutely. A professionally managed migration follows strict security protocols to ensure a HIPAA-compliant EHR system throughout the process. This includes encrypted data transfer, role-based access controls, audit logs, secure cloud or on-prem environments, and compliance-aligned validation checks. Security and compliance are embedded into every phase—from extraction to go-live—ensuring patient data remains protected at all times.
Winston Human Score: